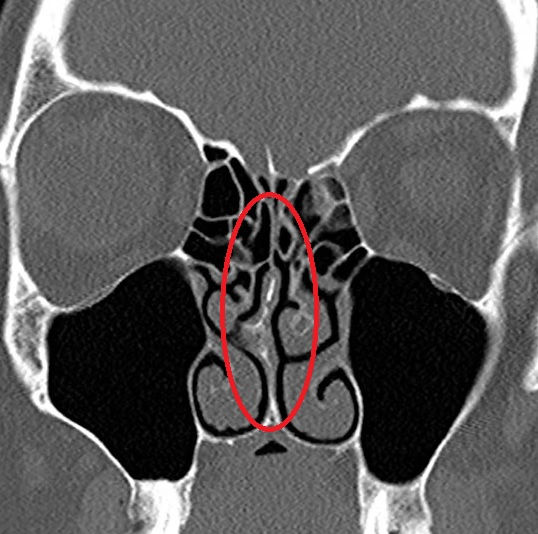
Turbinate Hypertrophy: Why Your Nose Feels Blocked Even Without a Deviated Septum
- 6 days ago
- 5 min read
Written by Mr Tim Biggs | Consultant ENT Surgeon | Rhinology & Facial Plastics
The Turbinates: What They Are and What They Do
Inside each nostril, three bony shelves project from the lateral nasal wall into the airway. These are the inferior, middle, and superior turbinates. The inferior turbinates are by far the largest and the most clinically significant. Covered in a layer of highly vascular mucosa, the inferior turbinates play a central role in nasal physiology: they warm and humidify inspired air before it reaches the lungs, filter out particles, and regulate the distribution of airflow across the nasal cavity.
The inferior turbinate mucosa is also dynamic. In a normal nose, the two inferior turbinates cycle through phases of relative engorgement and decongestion alternately, a process called the nasal cycle. This means that at any one time, one side of the nose is relatively more open than the other, though most people are unaware of this unless one side becomes pathologically enlarged.
What Is Turbinate Hypertrophy?
Turbinate hypertrophy refers to persistent enlargement of the inferior turbinates beyond normal physiological variation, resulting in narrowing of the nasal airway and symptomatic nasal obstruction. The enlargement may be mucosal, bony, or both. In chronic cases, the turbinate mucosa undergoes structural changes, including fibrosis and glandular hyperplasia, that mean it no longer responds normally to topical decongestants or even to nasal steroid sprays.
It is one of the most common conditions I see in rhinology practice, yet it is frequently missed or underemphasised by clinicians who focus solely on the septum when assessing nasal obstruction. In many patients, turbinate hypertrophy coexists with septal deviation, where the turbinate on the wider side of the nose compensates by enlarging, a phenomenon known as compensatory hypertrophy. Addressing the septum alone in these cases produces a disappointing result.
What Causes Turbinate Hypertrophy?
Several factors can drive persistent inferior turbinate enlargement:
• Allergic rhinitis, where chronic allergic inflammation causes mucosal thickening and vascular engorgement
• Non-allergic rhinitis, including vasomotor and irritant-driven patterns
• Compensatory hypertrophy secondary to septal deviation
• Prolonged use of topical decongestant sprays (oxymetazoline, xylometazoline), causing rebound mucosal swelling known as rhinitis medicamentosa
• Hormonal changes, including pregnancy and hypothyroidism
• Environmental irritants including pollution, tobacco smoke, and occupational exposures
Identifying and addressing the underlying driver is an important part of management. Surgery improves the airway, but if an allergic or irritant cause is not also managed, the hypertrophy is more likely to recur over time.
Symptoms of Turbinate Hypertrophy
The predominant symptom is nasal obstruction, which patients typically describe as a sense of congestion or stuffiness rather than a sharp blockage. Other commonly reported symptoms include:
• Bilateral nasal obstruction, that can alternate but cause complete blockage
• Worsening congestion when lying down, due to increased venous pooling in the turbinate mucosa
• Mouth breathing and snoring
• Difficulty sleeping due to nasal obstruction or persistent nasal blockage even after septoplasty surgery
• Reduced sense of smell
• Catarrh and postnasal drip
• Sensation of nasal congestion that does not respond to steroid sprays
Diagnosis
Diagnosis is made at nasal endoscopy. I use an endoscope to directly visualise the inferior turbinates, assess their size and character, and evaluate the rest of the nasal cavity. This takes only a few minutes in clinic and is well tolerated. Allergy testing may be arranged where allergic rhinitis is suspected as a contributing factor.
The endoscopic assessment allows me to distinguish between mucosal hypertrophy, which may respond to medical treatment, and bony hypertrophy with mucosal fibrosis, which typically requires surgery for meaningful and durable improvement.
Medical Treatment: What Works and What Doesn't
Nasal corticosteroid sprays are the first-line medical treatment for turbinate hypertrophy and are effective in many patients, particularly those with a significant allergic component. They reduce mucosal inflammation and can meaningfully reduce turbinate size when used regularly and correctly over a sustained period.
Antihistamines may provide additional benefit in allergic rhinitis. Saline nasal irrigation improves mucociliary clearance and reduces mucosal irritation. Allergen avoidance and, where appropriate, allergen immunotherapy address the underlying allergic drive.
However, in patients with chronic structural turbinate hypertrophy, particularly those with significant bony component or longstanding mucosal fibrosis, medical treatment provides incomplete and often temporary relief. Surgery is the most effective and durable option in this group.
Turbinate Reduction Surgery: My Approach
My preferred technique for inferior turbinate reduction is submucosal microdebrider turbinoplasty, performed under general anaesthetic. This approach uses a powered instrument inserted beneath the mucosal surface to remove the bony and soft tissue bulk of the turbinate from the inside, while leaving the mucosal lining intact.
Preserving the mucosal surface is important. The mucosa of the inferior turbinate is responsible for warming and humidifying inspired air, and over-aggressive turbinate surgery that strips away the lining can result in a nose that is dry, crusting, and paradoxically feels blocked despite being anatomically open, a distressing condition known as empty nose syndrome. My technique specifically avoids this by targeting the submucosal component while leaving functional mucosa in place.
The procedure takes approximately 20 to 30 minutes per side and is performed as a day-case. It is very commonly combined with septoplasty when both conditions coexist, which is the norm rather than the exception.
What to Expect After Surgery
Patients breathe through the nose immediately after surgery, which makes the immediate post-operative experience significantly more comfortable than aggressive and complete nasal packing.
The nose will feel congested for the first one to two weeks as surgical swelling settles. Nasal saline douching from the day after surgery keeps the cavity clean and supports mucosal healing. Most patients are back to normal activity within one to two weeks, with the full functional benefit of surgery appreciated by six to eight weeks.
Arrange a Consultation
If you have a persistently blocked nose that has not responded adequately to nasal sprays, I would be glad to assess you. Nasal endoscopy will identify whether turbinate hypertrophy, a deviated septum, or a combination of both is responsible, and we can discuss the most appropriate management from there.
I see patients privately. To arrange a consultation, please contact my secretary Michele Hewlett. Fees are available at www.hampshireentclinics.co.uk.

Frequently Asked Questions
What are turbinates?
Turbinates are bony shelves lined with mucosa that project into the nasal cavity. The inferior turbinates are the largest and most clinically significant, regulating airflow, warming and humidifying inspired air, and filtering particles.
What causes turbinate hypertrophy?
Turbinate enlargement is commonly caused by allergic or non-allergic rhinitis, environmental irritants, septal deviation causing compensatory hypertrophy on the wider side, or prolonged use of decongestant nasal sprays causing rebound swelling.
What is turbinate reduction surgery?
Turbinate reduction is a procedure to reduce the size of enlarged inferior turbinates to improve nasal airflow. Mr Biggs uses submucosal microdebrider turbinoplasty under general anaesthetic, which reduces bony and soft tissue bulk while preserving the mucosal surface.
Is turbinate reduction painful?
The procedure is performed under general anaesthetic. Post-operative discomfort is generally mild and managed with simple analgesia. There is no nasal packing, which makes recovery considerably more comfortable.
How long does recovery take after turbinate reduction?
Most patients return to normal activity within one to two weeks. The nose may feel congested initially as swelling settles, with the full benefit of surgery apparent by six to eight weeks.
Will my nose become too dry after turbinate reduction?
This is a concern with over-aggressive turbinate surgery. Submucosal microdebrider turbinoplasty preserves the mucosal surface and humidifying function, significantly reducing the risk of post-operative dryness or empty nose syndrome.
Where does Mr Tim Biggs perform turbinate reduction?
Mr Biggs performs turbinate reduction privately in Hampshire.
How do I find out the cost?
Fees are listed at www.hampshireentclinics.co.uk. To book a consultation, contact Michele Hewlett, Mr Biggs's secretary.